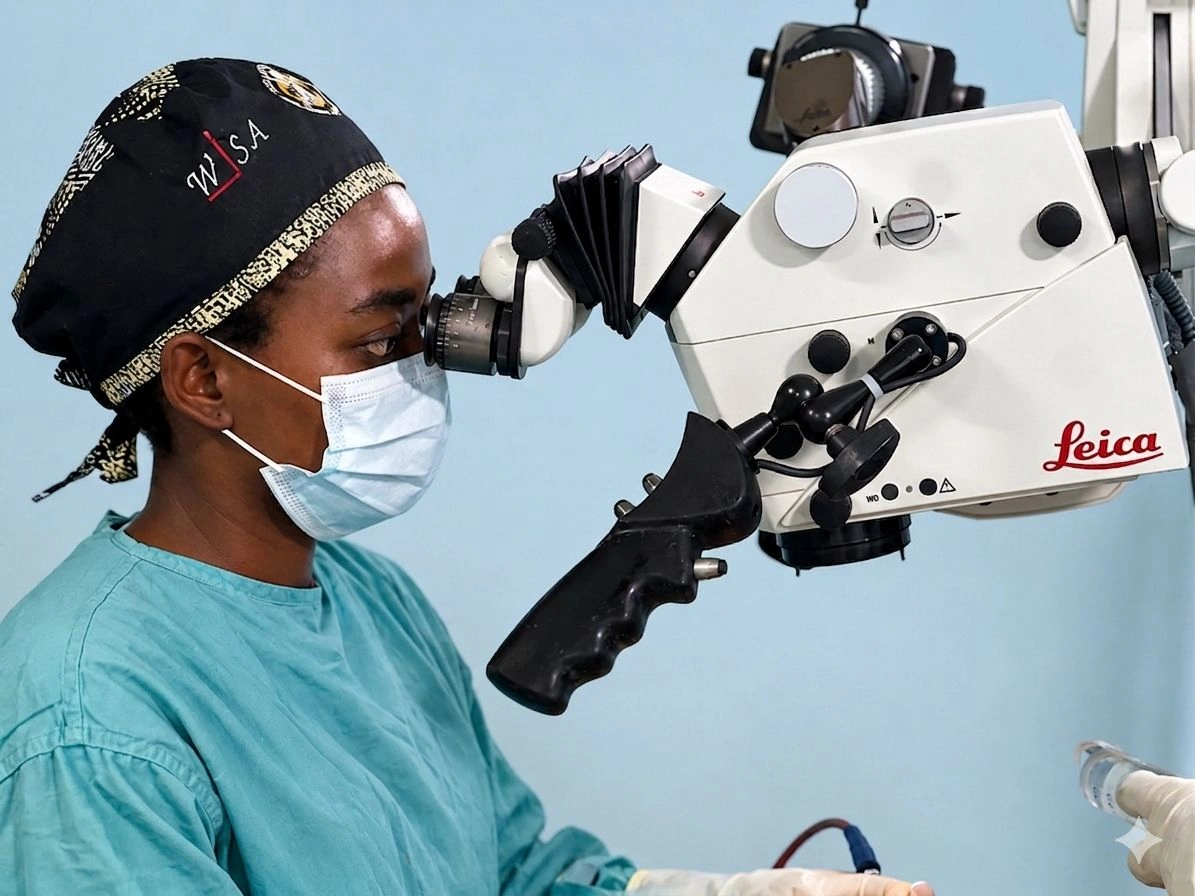
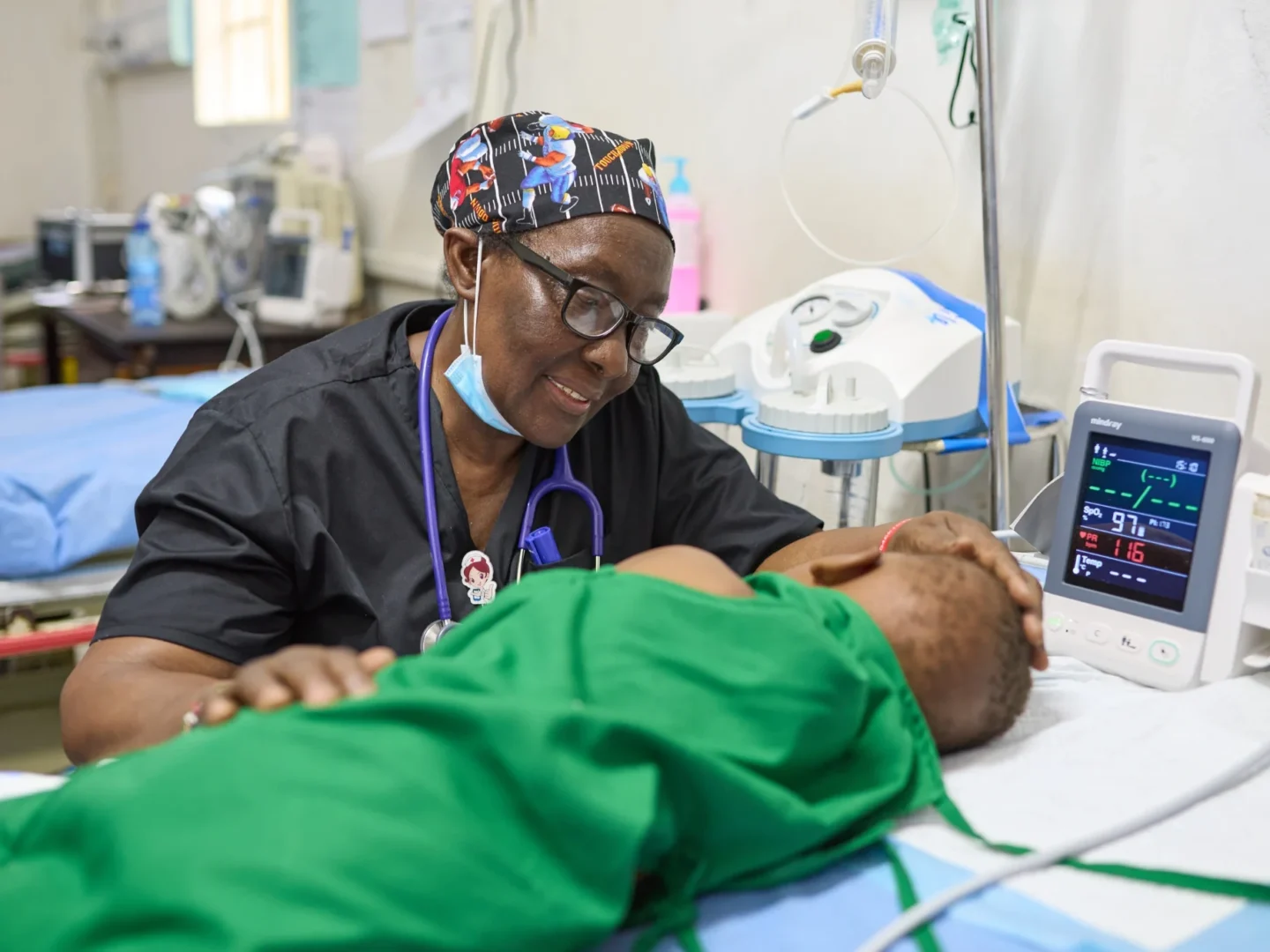
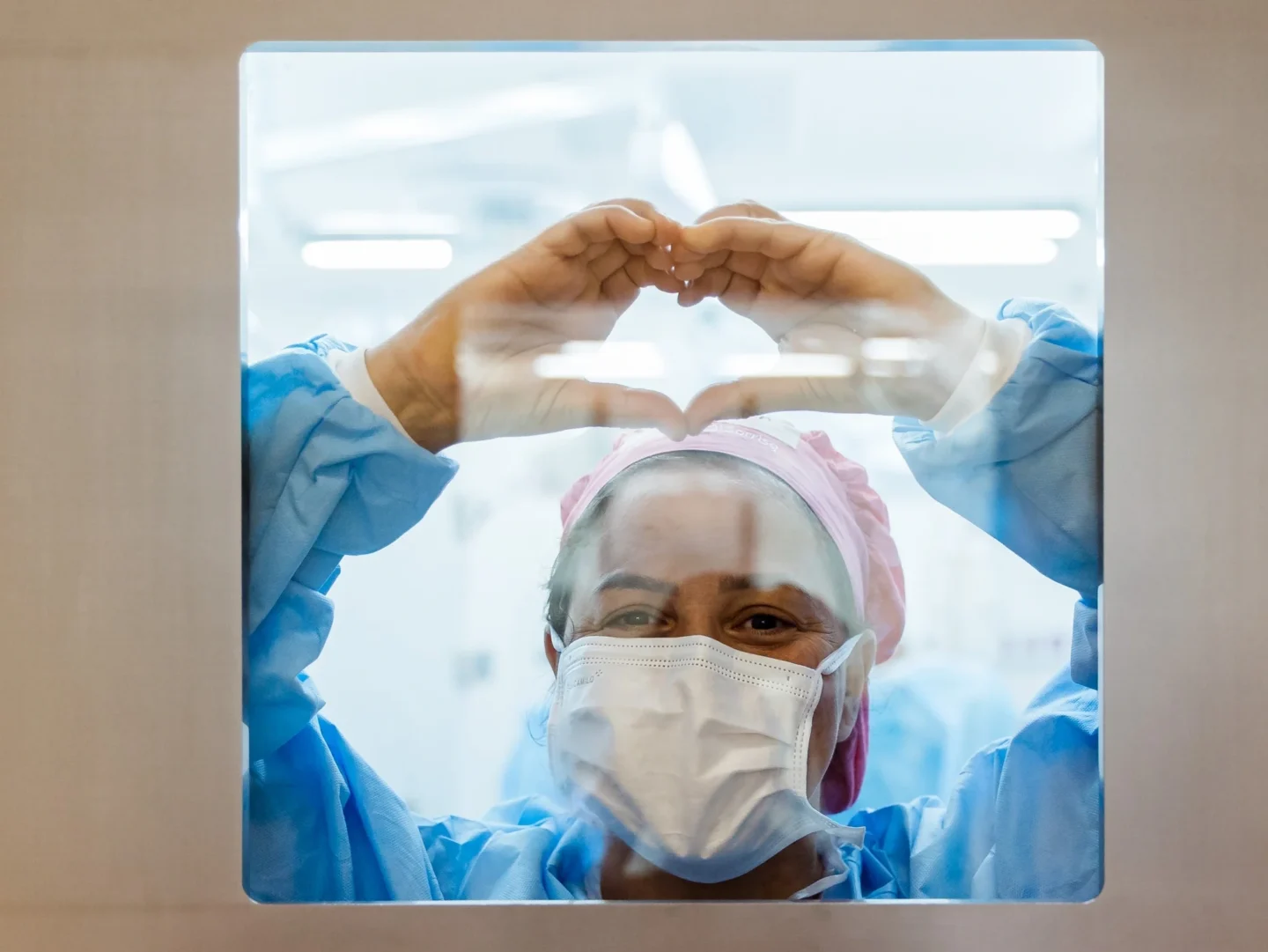
Care Providers
Celebrating World Patient Safety Day
We’re proud to join with the World Health Organization (WHO) and members of the health care community in celebrating World Patient Safety Day on September 17. According to WHO, this commemorative day “calls for global solidarity and concerted action by all countries and international partners to improve patient safety.”
For us, patient safety is our first priority every day. We’ve created robust medical standards, and we build teams with diligent and caring medical professionals to ensure the best possible outcomes for our patients.
To learn more about Operation Smile’s focus on patient safety, we caught up with Dr. Bryan Zimmerman, Operation Smile’s vice president of medical quality.

Q: What does your role as Operation Smile’s vice president of medical quality entail?
A: “I’m responsible for the overall planning, direction and operation of quality, risk management and patient safety. I serve as a member of Operation Smile’s senior leadership team and am responsible for the design and direct implementation of the organization’s Quality Assurance Program. In addition, I’m an expert in defining and implementing evidence-based medical quality systems and compliance standards.”
Q: Can you explain what patient safety is and why it’s important?
A: “The goal of patient safety is to minimize adverse events and eliminate preventable harm in health care. Patient safety is the fundamental use of methods and tools utilized to deliver quality essential health services such as cleft care. That being said, patient safety is more than a set of rules or directives; rather, patient safety is a culture and mindset that is driven from the top down.
“The Operation Smile leadership team is clear that quality health services around the world must be effective, safe and patient-centered. Ultimately, the benefits of patient safety yield quality health care. Patient safety integrated across health services is timely, equitable, integrated and efficient to ensure the best patient outcome.”
Q: Your team’s work in patient safety has a broader impact than on Operation Smile surgical programs alone. Can you provide an example of when Operation Smile patient standards have strengthened the local health system where we work?
A: “Abiy [Semunigus], the country manager of Operation Smile Ethiopia, put together a panel of medical professionals – surgeons, anesthesiologists, a biomed, nurse and pediatrician. That board, once a quarter, goes to a partnering hospital, bringing the form that the Operation Smile team created. This mobile-friendly form can collect first-hand observations and lag indicators from a patient’s chart. This information then becomes data that is visualized via PowerBI. The Ethiopian Minister of Health was so impressed with this product, they have adopted it. They absolutely love it.
“I also walked through Jimma University’s Pediatric ICU. We collaborated to develop a more refined space that would quickly identify any patient suffering a decompensation immediately, so we can provide the appropriate emergency response, as well as the equipment to provide those emergency, life-saving interventions. I worked with them on this for a year, and they recently cut the ribbon on the brand-new pediatric ICU.”
Q: How do you ensure patient safety after the patient leaves the surgical program?
A: “We’ve identified four pillars of safety: (1) proper screening of patient selection, (2) post-operative care, (3) emergency response and (4) discharge education. Discharge education is the one-on-one, heartfelt conversations between our nursing team and each patient and caregiver. They talk about things like the best way to provide medication, how to hold children when dispensing medication, what does feeding look like post-operatively, what does the diet look like, etc. They educate them on how to care for that freshly repaired surgical site, how to wash it, how to clean it, how to prevent infection and what to do in a variety of scenarios. These nurses set that parent up to be the next level of care and set them up for success.”
Q: How has our administration of surgical programs changed since early 2020, when COVID-19 was declared a pandemic?
A: “COVID reinforced that there was a significant opportunity within those local health care systems and health care workers [in the countries we work]. That led us to where we are today, with a significant interest in hospital-based partnerships. We have 186 [as of August 2023]. They serve in different capacities – some offer us space to conduct surgical interventions and operations, some of them provide ongoing care via surgeons or anesthesiologists who are affiliated with us and interested in providing cleft care between surgical programs. The pandemic really afforded us an opportunity to dig deeper, to get to some of those community and country backlogs, as well as educate and train future cleft surgeons, anesthesiologists, pediatricians and nurses. And finally, it allowed us the opportunity to strengthen or enhance those health systems through tools, communication efforts, education training, equipment support and more. We rely – for all the right reasons – on our local resources in-country, including our foundations – who are the true superheroes.”
Q: What does a surgical program look like now?
A: “Infection prevention is always a priority in our minds. We don’t want to set our staff members, caregivers or patients up for failure by neglecting any critical part of personal protective equipment. When parents come into the post-anesthesia care unit, and a child feels that hug or sit on mom or dad’s lap, it calms the child immediately. But we don’t compromise safety. We put the parent in a gown; we give them a surgical mask and put the booties on their feet. They are in a sterile area in the post-anesthesia care unit.
“The post-operative ward is a different type of space. We still emphasize hygiene and the proper ways to deliver medicine. We teach families antiseptic techniques to care for the patient, to keep that freshly repaired surgical site in the best possible condition.
“I have to tell you: It is nice to see faces again. For so many years, we didn’t get to see faces. You go home every day on a surgical program, and you know you made a difference that day because you got to see the faces of that parent and that child. There’s no greater satisfaction in the world than seeing the look in their eyes and the smile on their face.”
Q: What do you love most about the work you do?
A: “As a previous member of the military, I served in several combat deployments, conducting numerous direct-action missions. When I retired in 2017, I wondered where I would find that same sense of belonging and purpose as I had with my team. Operation Smile exceeded any expectation I ever had and has become a family that I am proud to be a part of.
“The best part of my position is to support our care teams while we provide hope, compassion and a drastically improved quality of life to the patients we serve. I vividly recall flying home from a country in battle and feeling an ache for the people of that country. With Operation Smile, every time I fly home from a program, my heart is full knowing the love and kindness that was poured into every encounter.”