Patients
Helping Heal Through Therapeutic Play
A Q&A with Psychosocial Care Provider Cathy Cheonga

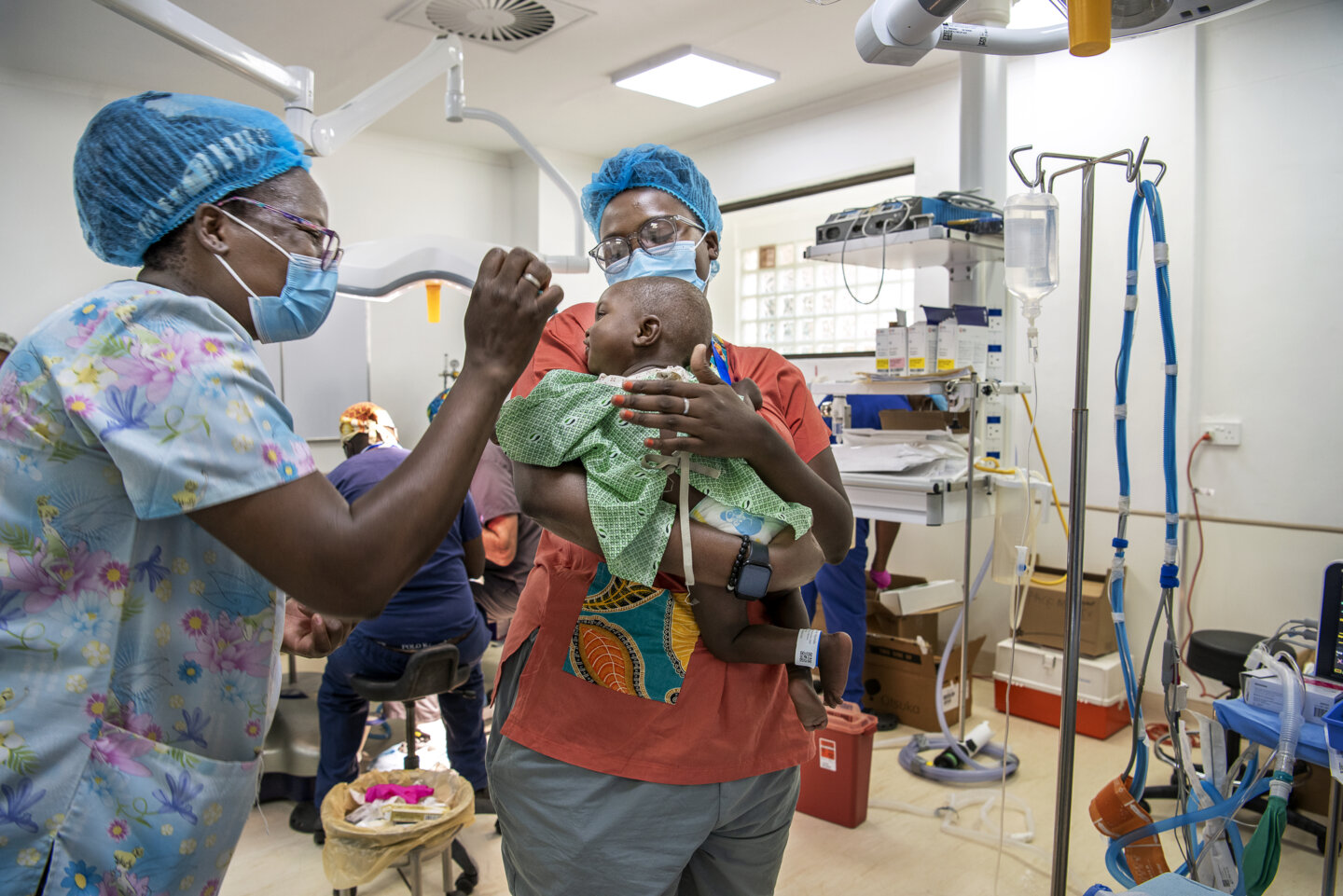
Local volunteers like Cathy Cheonga serve vital roles in the countries they work by delivering tailored care services to help families and patients thrive.
As a psychosocial care provider who has attended six Operation Smile surgical programs so far, Cathy uses therapeutic play and hands-on educational activities to help patients feel calm and prepared to enter the operating room. This aspect of comprehensive care has a major impact on children and families, many of whom have never been to a hospital or ventured outside of their communities.
“Everything is new to them,” Cathy said. “I love to work with the caregivers as well as the patients, just to reassure them and to tell them that there is hope, there is a smile at the end of the journey.”
With years of experience in connecting with patients in her home country of Malawi, Cathy has become attuned to the specific needs of those born with cleft conditions who may not see the challenging road ahead.
“Stigma is the biggest enemy,” she said. “Most of those patients who we are seeing are not going to school. Only a few are going far with education. So, stigma remains a big challenge.”
We caught up with Cathy to learn more about the challenging and rewarding aspects of her role as well as which memory of a patient stands out most in her mind.

Q: Tell us more about your role as a psychosocial care provider and your responsibilities on a surgical program?
A: “I support patients and caregivers from their first moments when they arrive on screening day. That’s the most important time to interact with the caregivers, as well as the patients. Because for most of them, they may have never been to the city or wherever we’re holding the surgical program. Everything is new to them. That’s the part where you become vulnerable so that they trust you. Then I help them and walk with them on the journey.
“Many are also scared because they’re being told stories about cleft conditions. For example, I met a mother whose child had a cleft palate, and in the village, that child has never been seen because people will tell them mean things like the child isn’t going to make it. This is the best part of the [program] because I love to work with the caregivers as well as the patients, just to reassure them and to tell them that there is hope, there is a smile at the end of the journey.”
Q: What is your favorite patient story?
A: “There are so many, but I still remember this one lady. She grew up in a village, and in that community, she was the only one with a cleft lip and palate. The stigma was really severe. However, her mother was determined to not give up on her. She used to say, ‘I’m going to keep this child!’
“She grew up into a young lady and got married, and they had two children together. One day, a friend of her husband told them that there were people providing care for people just like his wife. They were excited, but they were also concerned about how they could afford it, as they thought it would require a lot of money. Their friend told them that care was free and that they just had to register. He then got in touch with the patient coordinator, and they managed to get to the next surgical program.
“After surgery, she called me, and she said that she wanted to thank me for encouraging her. She told her husband that she wanted to go home very late so that they would arrive in the middle of the night so she could surprise all the ladies of the village the following morning. She said, ‘I knew they would be there watching and doing all the errands and they would be staring at me, genuinely surprised.’ I don’t think I’ll ever forget this story. She couldn’t believe that it was her when she looked at herself in the mirror. She thought it was a video. So I told her to go and look at her new smile on another mirror.”

Q: What are the biggest problems that you’ve seen affect the quality of our patients’ lives?
A: “Stigma is the biggest enemy. Because of that stigma, most of those patients who we are seeing are not going to school. Only a few are going far with education. But the rest, they might go to first grade or second grade. After that is when then they are likely beginning to experience bullying. When they are a bit older and they realize what is happening to them, they often decide to drop out from school. So, stigma remains a big challenge.”
Q: What can we do to help more children, especially from this psychosocial perspective?
A: “What I feel would help is to have mentors or psychosocial counselors being brought up in different communities where Operation Smile is so that they can be considered like support groups, helping the patients and families wherever they are coming from. This can have a great impact.
“We are losing a lot of children from education because they shy away from going back to school, and those parents can’t afford private tutors to be teaching those students at home. So these mentors can support them and maybe help the parents understand that the children can still go back to school with a cleft condition.”
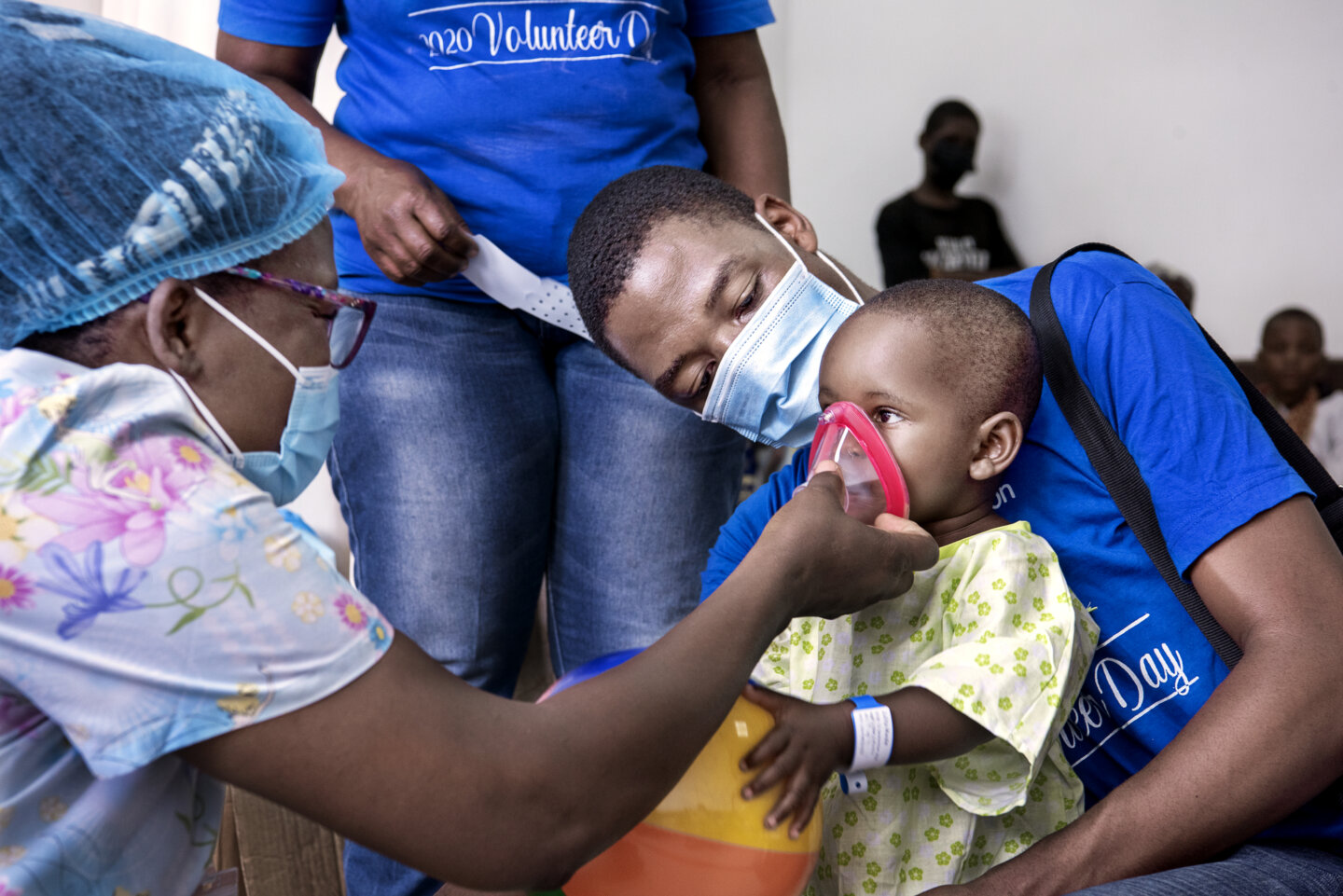
Q: What do you love most about working with Operation Smile? What are your hopes for Operation Smile Malawi specifically?
A: “There are so many professionals, medical and nonmedical, coming together and just giving it their all to create something special for the patients. I love the interaction and integrations. I’m also learning a lot of new things through working together.
“So my wish is to see that when children are born with cleft conditions, they’re attended to immediately. At that same time, bringing in different sectors. I know these people we’re bringing in. Most of them have the passion, and if they helped or were mentored so that they could see what is lacking in our nation, that would be great.”