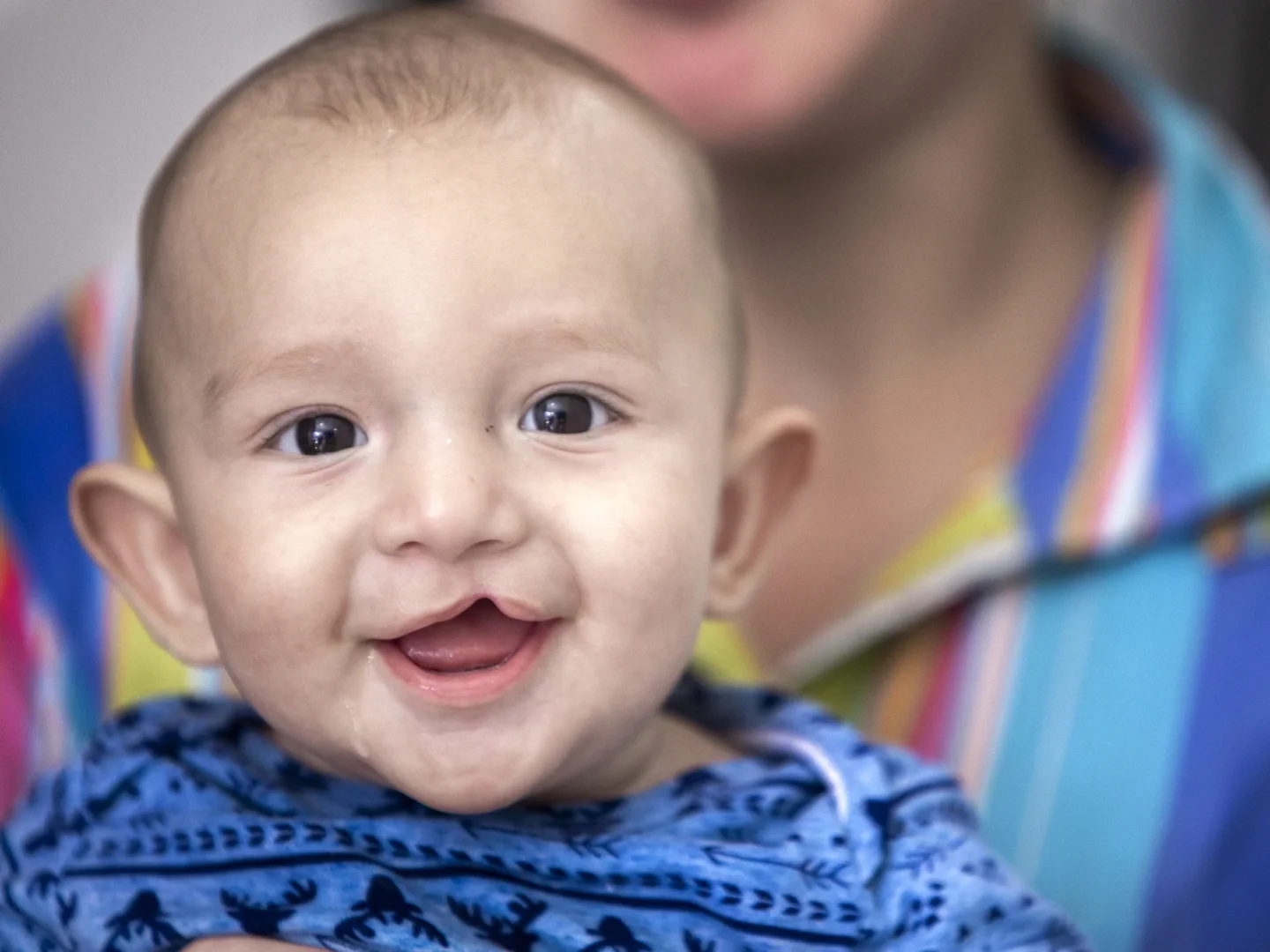
Patients
Completeness of Care: Psychosocial Care Providers

Out of sheer necessity, medical environments are controlled environments.
Sterility and a vast array of medical devices – from procedural instruments to monitoring systems – are critical to ensure the best possible patient outcomes.
Operation Smile care centers and surgical program sites are no exception.
The unintentional results are environments that can also evoke the nonmedical definition of “sterile” – stark and uninviting.
They can also strike fear and anxiety in young patients and their families, some of whom have never before stepped foot inside a medical facility.
Understanding that patients’ and their families paths to cleft surgery are often emotionally overwhelming, Operation Smile leans on the help of volunteer psychosocial care providers in the care center and surgical program settings.
These certified professionals provide psychosocial care and educate patients and their families about the entire surgical experience, easing their fears and anxieties through therapeutic play and activities.
“(Psychosocial care providers) guide children through developmentally-appropriate activities to help them gain mastery and control over their situations,” said Kelly Raymond, a child life specialist from Canada. “Children coming into the hospital don’t get to wear their own clothes, eat what they want or see what they want. (Our work helps give) them a piece of control over their environment.”

For many children, medical equipment like anesthesia masks – or even just being in a hospital – can appear to be ominous.
Psychosocial care providers use these devices as props during therapeutic play sessions so that patients won’t be surprised or frightened when those same surgical tools are used during their procedures. They also use this play time to help nervous parents understand what they can expect through every phase of the surgical process.
The psychosocial care area is also a place where silliness and fun is encouraged through age-appropriate play and activities, allowing kids to just be kids amid the stressful and unfamiliar environment.
“Receiving surgery can be a potentially frightening experience – (young patients) are exposed to strangers wearing strange clothes in a strange place. Play helps to normalize the health care experience for kids,” said Robert Wing, a volunteer psychosocial care provider.
“It empowers kids and gives them coping skills. Some of the kids leave the [surgical program] saying they had a fun time. That’s a powerful shift from being scared and frightened.”

The positive effects for children go beyond preparation for their individual procedures, explains certified child life therapist Sandy Forseth.
“In the playroom, children are seeing other children with their condition. They’ve been shunned or shamed by other people in their communities, so I think there is positivity when they get to meet other kids with cleft lip and cleft palate,” Sandy said.
She added: “From being a certified child life specialist, I’ve seen research that shows that when children are prepared ahead of time, they heal faster because they know what to expect.”

Building trust between children, families and the program or care center team is another key function of psychosocial care providers.
Kelly recalled a challenging but also rewarding experience from a program to Ethiopia in which her skills were tested by a fearful child.
“She clung tightly to her mother while crying and wouldn’t make eye contact with me. Teaching children about what to expect when they go in the operating room is our priority, but without trust, this can’t be done,” Kelly said. “Instead, I pulled out two wind-up toys and positioned them on the ground so they could race. She slowly started to peer out as the ladybug toy went in circles and the giraffe wind toy hopped along.
“The girl started to laugh. When they finished racing, the girl looked at me, expectantly. So I wound the toys up again, setting them on another race. This time, the girl sat up so she could watch the path the toys took. After a few more wind-up toy races, the girl crawled off of her mom’s lap, and she started winding up the toys herself.
“Eventually, I was able to teach her about the anesthetic mask. We practiced blowing bubbles and then blowing up a balloon with the anesthetic mask. She proudly showed her mom what she learned and even brought the mask over to her so she could try.
“When it was her time to go in for surgery, she held my hand as we walked down the hallway into the operating room. That simple act of play can change a child’s perspective and lead to empowerment and confidence. It’s situations like this that keep bringing me back to Operation Smile [surgical programs].”