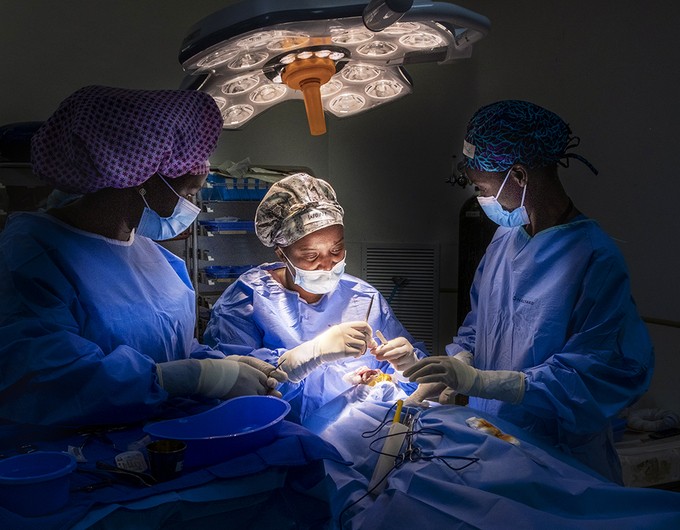
Our promise of improving health and dignity during the COVID-19 pandemic endures. We're helping front-line health workers stay safe, nourished and empowered to better serve their patients by providing life-saving supplies and equipment, as well as remote training to bolster their response. We’re also providing nutritional assistance, hygiene kits and virtual health services to support people and their health needs so they can thrive. If you can, when you can, help us keep our promise to care for children and create hope for tomorrow.
Although she’s devoted the last 36 years of her life to nursing, nothing prepared Victoria Leal for the day when a floor of her Florida hospital transitioned into a COVID-19 intensive care unit in less than 24 hours.
Born in Colombia, Victoria moved to the U.S. shortly after graduating and became an Operation Smile volunteer in 2011. Since then, she has donated her time, passion and skill as a pre- and post-operative nurse on 24 medical missions around the world.
Today, she’s dedicating her knowledge and skillset to serve and care for patients affected by COVID-19.
On March 13, during a routine team huddle at the start of her shift, Victoria and her fellow nurses sensed the initial effects of the coronavirus pandemic as members of their team began hectically preparing to admit a patient who would later become the first of many confirmed cases admitted into the hospital.
“I came back three days later. When I came back, everything was completely different,” Victoria said, recalling the events that followed that shift. “We never expected this.”
Like many medical professionals around the world responding to the events that are unfolding in their respective countries, Victoria combats these uncertain times by going beyond the call of duty for her patients, her team and her community.
We recently sat down with Victoria to learn more about how being an Operation Smile volunteer helped prepare her to face COVID-19 in her own country and to hear why she believes it’s vital to respect and recognize those who are on the front lines.
Q: Can you describe the series of events that started on March 13, with your team receiving two suspected positive patients, that led to your floor becoming a COVID-19 response unit in less than 24 hours?
A: “I was impressed, and I was scared also. I was impressed that everybody moved around very quickly, but I was scared for us. That was my extra shift. When I came into work that night, I was in the team huddle and the secretary came and started to clean everything faster. And he said, ‘We have two patients with COVID-19. We have two patients with COVID-19.’
“Everyone was looking at each other. Everyone’s behavior was different – scared. Another nurse who works with me said, ‘We have two patients. We have new scrubs for you. You have to change your gown, your scrubs, your uniform. You have to take a shower.’ Later, around 4 in the morning, there was another admission, a possible patient with COVID-19. I came back three days after that. When I came back, everything was completely different.
“You become very aware of how you move, everything that you do in the patient’s room so you don’t put yourself at risk to get the virus. You pay more attention on how you put on your mask, how you put on your gloves, how you put on your gown, how you remove everything before leaving the room. You move slow and try to be conscious of every movement.”
Q: How has being involved with Operation Smile helped prepare you for responding to the COVID-19 pandemic?
A: “I have been on 24 missions in different countries. My first mission was in Nicaragua. I’d never seen a poor place like this one, where they don't have any resources, where they don't have supplies. I think that the experiences in all those countries that don’t have what we really need, the basic stuff, teaches you to be more creative. It teaches you to have more of an imagination to create something to survive, to protect yourself or to work with a patient because we learn from those nurses who work with such limitations. They made me more compassionate. I have experience from different countries with how people deal with situations without resources and how they live.”

Q: What limitations have you and other members of your team faced?
A: “When we go to the patient's room, we're supposed to use an N95 – it’s the special mask that has a filter. This mask is supposed to be disposable. We're supposed to use it one time with one patient and throw it away. Then we use a gown that's supposed to be thrown away after one entry to the patient’s room. We have to recycle them. We use double gloves. We use shoe protectors. We also use a surgical hat.
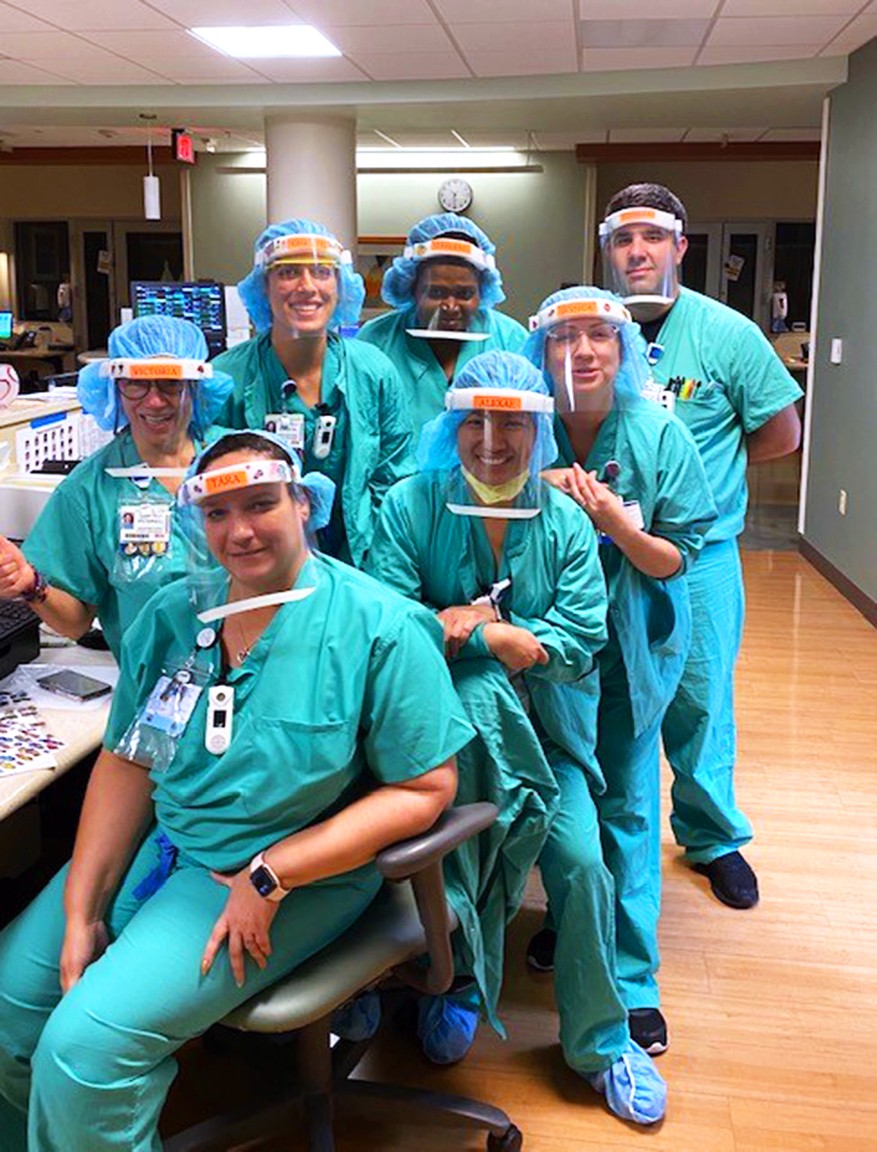
“This is what we need. But we are short of gowns. We are short of N95s. We are short of surgical masks. We don't have any more shoe covers. We recycle. I’m making face shields for my coworkers because we don’t have enough. We never expected to be running out of these supplies that we once threw away every single day.”
Q: In light of this pandemic, why do you feel it’s so important to recognize nurses and the role they serve in the medical field?
A: “We are the first responders. We are first responders for everything. We see that the life of the patient is in our hands. We have more contact with the patient. We are who see the patient in a whole picture. We are the ones who have the privilege to take care of all human beings completely.
“In this pandemic, it's more. We have to deal with respiratory problems and act and do something to keep those alive. We are giving direct care to the patient 24/7. We are exposed, we are afraid, but we are brave and ready to do our job.”
Q: What are your thoughts on how this virus seems to affect people of all ages with various medical histories?
A: “We always talk to each other about how differently this virus attacks people. It’s difficult to say who’s going to be released or who is going to get sicker. I had one lady, 84 years old, who was positive with no symptoms at all. None. No pain, no shortness of breath. Another one, 56, is fighting to be alive. It’s scary because we don't know how we fight with something that we don't understand. We don't have information, clear information, about this virus. That’s really surprising for everybody every day. Every day is different.
“It can be somebody's uncle, it can be your mom, your brother, your son. It can be anyone. It doesn't matter. Black, white, Hispanic, American. It doesn't matter how much money you have. It doesn't matter at this point. That patient could be my co-worker, could be my husband, could be my son, could be my mother. This touches everybody.”
Q: What motivates you to continue fighting on the frontlines?
A: “Yesterday, I was reading an email from the daughter of one of my patients. It was a thank you letter about the staff who was with the patient and everything that we did for the patient. Her father was a patient who died. The daughter said that she really appreciates what we do in my unit in this difficult moment. She made a donation to my unit. And she asked, ‘Why are you there? What is it that keeps you working in this?’
“One of my other patients once said, ‘You saved my life yesterday. I was sick and you saved my life.’ This is the situation. Sometimes it's good, sometimes it’s bad, but that keeps you going. When a patient goes home. When the patient gets better. When we work so hard with the patient and in the morning the patient is stable.
“I told the other nurses, ‘Don't go work for a check. Please don't go for a check. You go to take care of the patient and to be motivated with the results.’ I think that with this pandemic, nurses feel or think that they need to be better nurses.”

Latest Stories

A Former Patient, Aymane Now Shares His Story

What is Operation Smile's Nutrition Program?