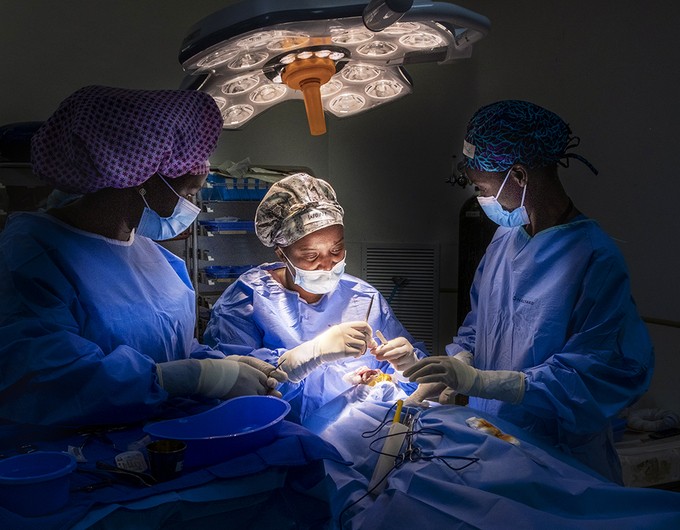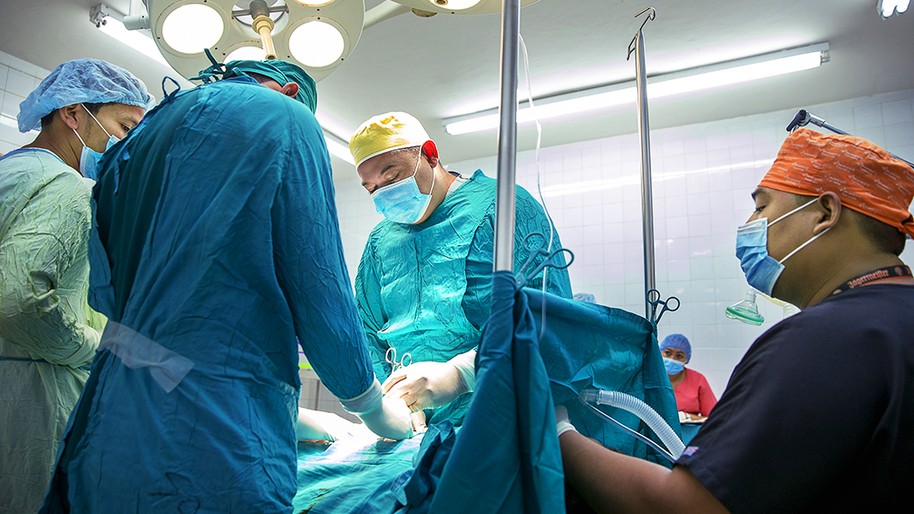
A single-engine Cessna 208 Caravan is filled to the brim with passengers and luggage, making its way through the clouds, up and away from the busy city of Managua toward Nicaragua’s northeast.
Soon, Lake Managua and the characteristic volcanoes are out of sight and sprawling beneath are hills, rivers, forests and a few scattered villages surrounded by farmland.
An hour later, the propeller plane lands on a strip of gravel in the middle of the town of Bonanza. This is Nicaragua’s Mining Triangle, a remote and rural area known for its mineral resources. Two other towns create the corners of the triangle – Siuna to the south and Rosita to the west.
Here, with support from the UBS Optimus Foundation, Operation Smile and Nicaragua’s Ministry of Health are working together on a pilot project at the two primary hospitals in Siuna and Bonanza called Cirugía para el Pueblo – “Surgery for the People.”
By joining forces, Operation Smile and the Ministry of Health seek to improve the surgical infrastructure of the hospitals and to spread awareness about surgically-treatable conditions to the people of the region.

“Part of the background is what is happening in the world, where more people die from conditions that are treatable by surgery than by HIV, malaria and tuberculosis combined,” explains Dr. Jordan Swanson, the now-former director of surgical innovation and special programs with Operation Smile, a plastic surgeon from the United States who led the project.
It all began when Jordan and his colleagues at Operation Smile travelled to the Mining Triangle to search for people with untreated cleft conditions. Many people in this region live in very remote villages; the closest main road could take hours to reach by walking or by riding horseback, followed by a bus ride of several more hours to reach their primary hospital.
While spending time at the hospitals there, the Operation Smile team got to know the surgeons and anesthesiologists and saw how dedicated, skilled and committed they are, despite working with very limited resources.
“It struck me that this was a great opportunity for us to partner together with the ministry and really figure out how safe surgery is possible also in an area like this,” Jordan says. “Many people think of us as a cleft organization; we take care of kids with cleft. I think one can also think of Operation Smile as an organization that achieves high-quality surgical care. We have more than 35 years of experience figuring out how to create impact and get the job done at the end of the day.”
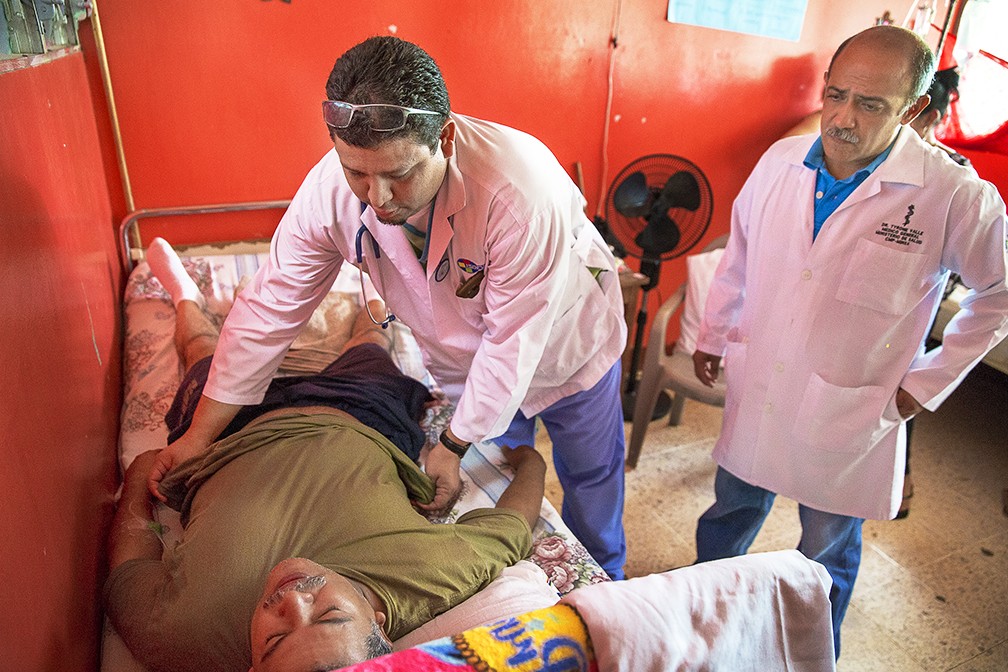
And this is where Operation Smile can play an important role in public health.
A few years ago, the Lancet Commission on Global Surgery showed that more than half of the global population lacks access to safe and affordable surgical care when they need it, such as when someone experiences bleeding after childbirth, suffers a burn, develops cancer or is born with a cleft condition. More than 143 million surgical procedures are needed – mostly in low- and middle-income countries like Nicaragua – to save lives and prevent disability, around 5,000 procedures per 100,000 of the population.
“Well, this is very straight forward. In places like Siuna and Bonanza, only about 20 percent of the people in the region are getting the surgery they need,” Jordan says. “Many of them are referred to the capital city hospitals, and that is a tough trip to make and many aren’t going to make it.
“Now, how do we get to the rest of those patients? Part is education, part is equipment and supplies, and part is thinking through how we can connect to the patients and the community and then how to follow up on the outcomes.”
At Hospital Primario Esteban Jaenz Serrano in Bonanza, the problem is tangible. Even though in recent years the hospital has been renovated and refurbished, director Maria Isabel Flores Johnson still has a long list of needs – one being to open another operating theatre. With only one operating room, scheduled surgeries have to give way to emergencies, forcing people to wait for days or weeks. The time spent away from work or family can cause both stress and economic problems for the patient.

Improved human resources is another need with the most imminent being the lack of an anesthesiologist.
“We haven’t been able to hire one because after they finish university, they don’t really like to come here to work,” Maria says. “They want to have a higher salary, better conditions and more benefits.”
Yadive Ríos is an anesthesia technician and the only person at the hospital qualified to provide anesthesia. However, the services she is able to provide are limited.
“I can’t help out on pediatric or geriatric surgery, so if we, for example, have an 80-year old patient, he or she needs to be referred to another hospital, which means sometimes travelling almost 400 kilometers to Managua in order to get surgery,” Yadive says.
This also means that whenever Yadive has to miss a day of work, the hospital is forced to cancel surgeries.
“I am the only one here on the staff to do this and they need me, so I ask myself how ill I am on a scale from one to 10, and if I have a fever or a flu, I still go to work,” Yadive says. “But everyone in this hospital makes these kinds of efforts. We are a small hospital and the population has increased a lot these last years, so it is difficult, it can be very dense.”
Yadive shows us the operating ward, where the entire water piping system is to be upgraded to a new and modern one. Cosponsored by a local mining corporation, it will be the first renovation of the Surgery for the People project.
By hand, she turns on the faucet where the surgeons wash their hands before surgery. In most operating rooms, faucets are operated by doctors’ feet or knees to make sure their hands remain as sterile as possible. Worse, the water that comes out of the tap is brown and full of mud.
“Our problem with the water is not just that it is unhealthy and not drinkable, but also sometimes that there is no water at all,” Yadive exclaims. “Because it comes directly from the river, it is not cleaned in a water plant, and sometimes there is so much mud in the water that it plugs the entire system.”
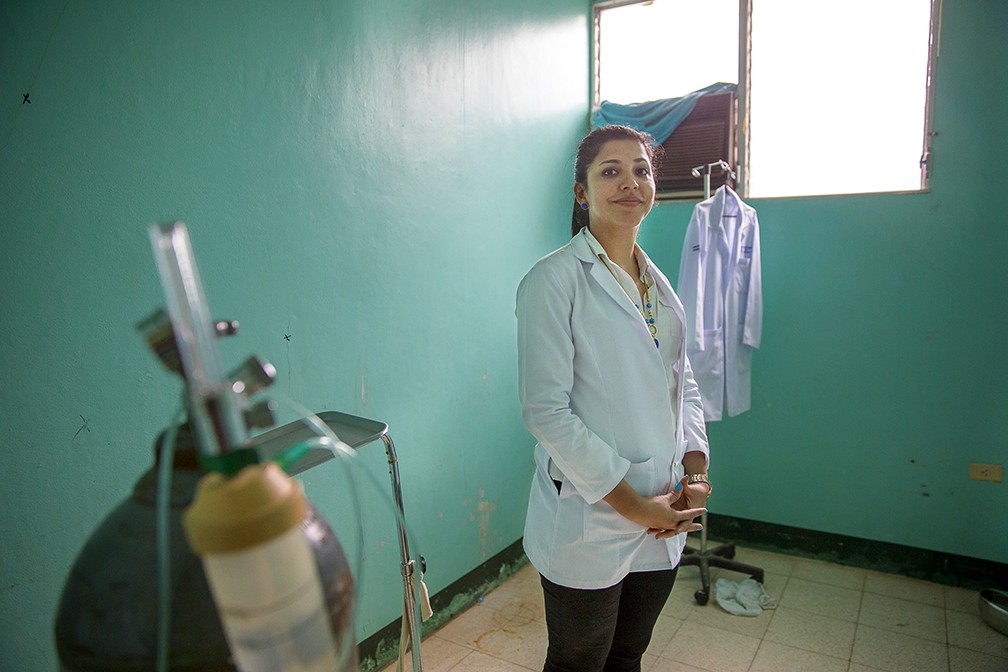
At Hospital Carlos Centeno in Siuna, the situation is just as bad. The lack of proper surgical equipment, operating theatres and staff means that delays and cancelled surgeries are common. Patients who have travelled for days often have nowhere to stay because of lack of beds and wards. Many also arrive with acute illnesses that turn deadly because they never knew that their ailment could be treated by surgery.
“If someone ignores what is an infected appendix, believing it is a parasite, this person will die. It is no one’s fault, it is just the lack of knowledge,” says Dr. Tyrone Valle, a general surgeon at the hospital.
He’s very excited about the project and the education and awareness it will bring for the hospital staff and the community alike. For example, a manual of surgical diseases is being developed, in which the most common surgical diseases are outlined. These manuals will be used at the local health clinics in the remote villages, so people will be able to understand that their condition can be cured by surgery – as long as they visit a doctor as soon as they experience symptoms.
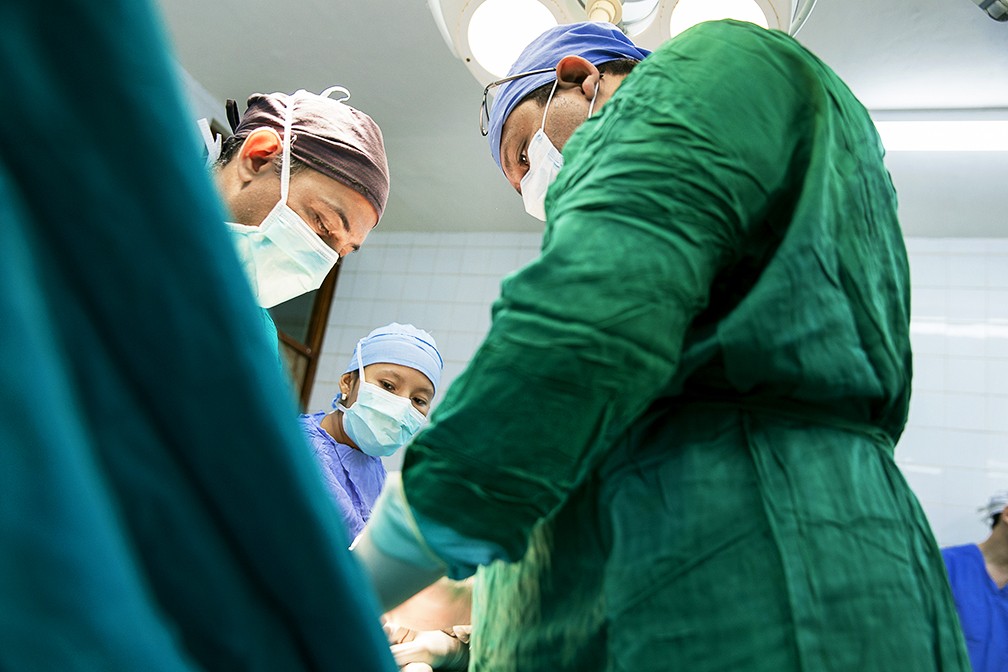
“When I first came here 20 years ago, we were 20 employees. At that time, there were still armed conflicts here and we received many patients with injuries from guns and pistols, in the stomach or thorax, and injuries by knives because of conflicts over land,” explains Tyrone. “Now, there are almost 200 working here and we have peace in the country, so the causes of death have changed. We don´t have to treat wounds but instead diseases that are curable by medicine or surgery. So, this project can really help people, just by giving them the message that we can treat them and educate them as long as they will come here in time for surgery.”
Latest Stories

A Former Patient, Aymane Now Shares His Story

What is Operation Smile's Nutrition Program?